Jugular venous pressure
Revisione paritaria di Dr Laurence KnottUltimo aggiornamento di Dr Colin Tidy, MRCGPUltimo aggiornamento 20 Dic 2021
Rispetta le linee guida editoriali
- ScaricaScarica
- Condividi
- Language
- Discussione
- Versione audio
- Add to preferred sources on Google
Professionisti Medici
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our articoli sulla salute more useful.
In questo articolo:
Continua a leggere sotto
What is jugular venous pressure?
Jugular venous pressure (JVP) provides an indirect measure of central venous pressure. The internal jugular vein connects to the right atrium without any intervening valves - thus acting as a column for the blood in the right atrium. The JVP consists of certain waveforms and abnormalities of these can help to diagnose certain conditions1 . Unfortunately, detection of these abnormalities and even the JVP itself, can be difficult and has also been superseded by other diagnostic methods.
How to examine jugular venous pressure1
Torna ai contenutiUse the right internal jugular vein (IJV).
The patient should be at a 45° angle.
The patient's head should be turned slightly to the left.
If possible, have a tangential light source that shines obliquely from the left.
Locate the surface markings of the IJV - this runs from the medial end of the clavicle to the ear lobe, under the medial aspect of the sternocleidomastoid.
Locate the JVP - look for the double waveform pulsation (palpating the contralateral carotid pulse will help).
Measure the level of the JVP by measuring the vertical distance between the sternal angle and the top of the JVP. Measure the height - usually less than 3 cm.
Continua a leggere sotto
Waveforms of jugular venous pressure
Torna ai contenutiJugular venous pulse
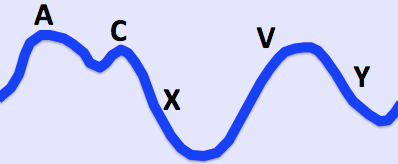
© By Ecgtocardiology, via Wikimedia Commons
Informazioni importanti |
|---|
Waves1 un - presystolic; produced by right atrial contraction. c - bulging of the tricuspid valve into the right atrium during ventricular systole (isovolumic phase). v - occurs in late systole; increased blood in the right atrium from venous return. Descents x - a combination of atrial relaxation, downward movement of the tricuspid valve and ventricular systole. y - the tricuspid valve opens and blood flows into the right ventricle. |
The a and v waves can be identified by timing the double waveform with the opposite carotid pulse. The a wave will occur just before the pulse and the v wave occurs towards the end of the pulse. Distinguishing the c wave, x and y descents is an almost impossible task.
How to differentiate a jugular venous pulse from the carotid pulse
Torna ai contenutiThe jugular venous pulse is:
Not palpable.
Obliterated by pressure.
Characterised by a double waveform.
Variable with respiration - it decreases with inspiration.
Enhanced by the hepatojugular reflux (see below).
Continua a leggere sotto
Hepatojugular reflux (abdominojugular reflux sign)2
Torna ai contenutiThis can help to confirm that the pulsation is caused by the JVP.
In the classic test for hepatojugular reflux, firm pressure is applied to the right upper quadrant using the palm of the hand. It has been realised that pressure anywhere over the abdomen will produce the same result (abdominojugular reflux sign). Pressure over the peri-umbilical region is the usual method and may be more appropriate in patients with a tender liver.
A transient increase in the JVP will be seen in normal patients.
There may be a delayed recovery back to baseline which is more marked in right ventricular failure.
Raised jugular venous pressure causes
Torna ai contenutiInsufficienza cardiaca.
Constrictive pericarditis (JVP increases on inspiration - called Kussmaul's sign).
Cardiac tamponade.
Fluid overload - eg, renal disease.
Superior vena cava obstruction (no pulsation).
Jugular venous pressure abnormalities1 3
Torna ai contenutiAbnormalities of the a wave
It disappears in atrial fibrillation.
Large a waves occur in any cause of right ventricular hypertrophy (pulmonary hypertension and pulmonary stenosis) and tricuspid stenosis.
Extra large a waves (called cannon waves) in complete heart block and ventricular tachycardia.
Prominent v waves
Tricuspid regurgitation - called cv or v waves and occurring at the same time as systole (a combination of v wave and loss of x descent); there may be earlobe movement.
Slow y descent
Tricuspid stenosis.
Right atrial myxoma.
Steep y descent
Insufficienza ventricolare destra.
Pericardite costrittiva.
Tricuspid regurgitation.
(The last two conditions have a rapid rise and fall of the JVP - called Friedreich's sign.)
Prognostic use of jugular venous pressure
Torna ai contenutiElevated JVP in patients with heart failure is associated with an increased risk of hospital admission, death and subsequent hospitalisation for heart failure4 . Therefore, appreciation of this sign can be clinically helpful.
Ulteriori letture e riferimenti
- Chua Chiaco JM, Parikh NI, Fergusson DJ; The jugular venous pressure revisited. Cleve Clin J Med. 2013 Oct;80(10):638-44. doi: 10.3949/ccjm.80a.13039.
- Brostoff JM; Re-examining examination: misconceptions in clinical medicine. J R Soc Med. 2009 Jan;102(1):11-5. doi: 10.1258/jrsm.2008.080330.
- Witteles R; Neck Veins & Wave Forms, Stanford Medicine 25
- Drazner MH, Rame JE, Stevenson LW, et al; Prognostic importance of elevated jugular venous pressure and a third heart sound in patients with heart failure. N Engl J Med. 2001 Aug 23;345(8):574-81.
Continua a leggere sotto
About the author

Dr Colin Tidy, MRCGP
Medico di base, Autore medico
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Laurence Knott
Medico di base, Autore medico
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
Storia dell'articolo
Le informazioni su questa pagina sono scritte e revisionate da clinici qualificati.
Prossima revisione prevista: 19 Dic 2026
20 Dic 2021 | Ultima versione

Chiedi, condividi, connettiti.
Esplora le discussioni, fai domande e condividi esperienze su centinaia di argomenti di salute.

Non ti senti bene?
Valuta i tuoi sintomi online gratuitamente